There are three main reasons why disputed paternity and maternity cases are used in forensic sciences.
- When the child is born after marriage, but the husband denies fathering and seeks divorce.
- When a child is born outside a legal marriage, and the mother accuses a particular man as father, while the man denies the accusation.
- Child support cases of adoption or providing financial support to guidance.
Following are the tests and techniques used in solving disputed paternity and maternity cases involving legal systems and forensic evidence.
1. ABO Blood Group System
Human blood type is predetermined by particular GENES that we inherit from our parents.
These genes produce AGLUTINOGENS, which are found on the surface of all of our red blood cells. And these molecules determine our blood type.
Blood type is determined by three alleles or genes: A, B, and O. There are 6 possible combinations with two genes.
| ABO Blood Type | Possible Combination |
|---|---|
| Type A | AA or AO |
| Type B | BB or BO |
| Type AB | AB |
| Type O | OO |
| Blood Group | Antigen in RBC | Antibody in Serum | Approx Population (%) |
|---|---|---|---|
| A | A | Anti -B | 22% |
| B | B | Anti -A | 33% |
| AB | A & B | – | 05% |
| O | – | Anti -A & Anti-B | 40% |
In a blood group, the antigen cannot appear in a child unless, it is present in one or both parents, according to Mendelian principles, which govern how blood groups are passed down via families.
If a person has the homozygous form of a blood type factor, it must also be present in the blood of all his offspring.
If a child is homozygous for a factor, both of their parents may have contributed the gene.
The properties of the blood group are unique to the individual and remain unchanged over time.
Table of ABO Blood Group Possibility of Child Vs Parents Blood Group
| Parents | Child (possible) | Child (impossible) |
|---|---|---|
| A x A | A and O | B and AB |
| A x B | A, B, O and AB | None |
| A x AB | A, B and AB | O |
| A x O | A and O | B and AB |
| B x B | B and O | A and AB |
| B x O | B and O | A and AB |
| B x AB | A, B, and AB | O |
| AB x AB | A, B, and AB | O |
| AB x O | A and B | O and AB |
| O x O | O | A, B, and AB |
How to ABO Typing works in Solving Paternity Cases?
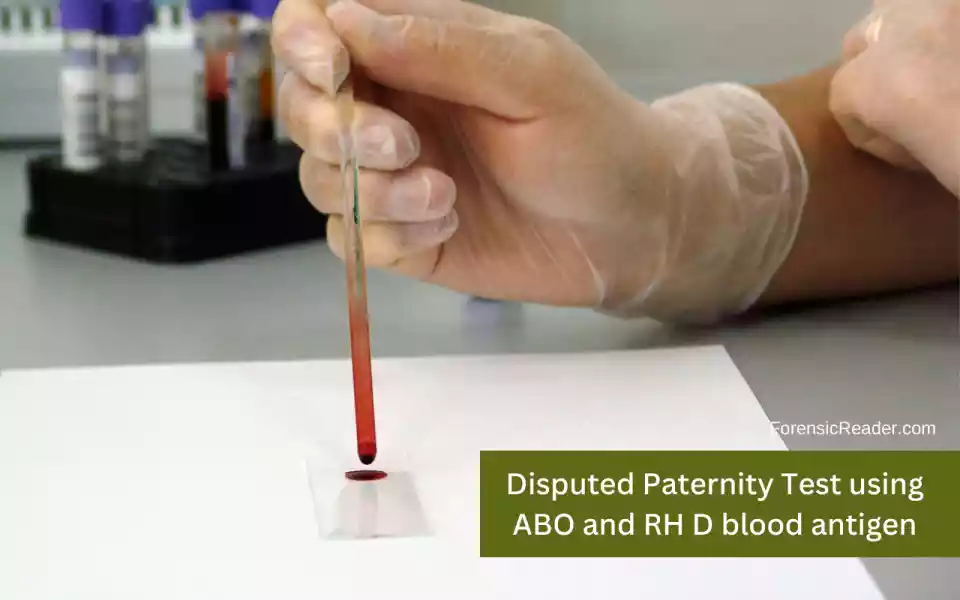
Principle:
- Type A blood contains naturally occurring anti-B antibodies that agglutinate only with B cells.
- Likewise, type B blood agglutinates only with A cells
- Type O blood agglutinates with both A and B cells
- Type AB blood does not agglutinate with any cells.
This result forms the basis for blood group typing.
Procedure (Slide Method):
- Divide a glass slide or white porcelain support into three parts. Label it as A, B, and O.
- Mix a drop of donor or recipient blood with anti-A, anti-B, and anti-D individually in each section.
- The ABO and rhesus D (RhD) types of blood can be identified visually from the pattern of blood clumping, or agglutination.
- This test takes only a small amount of blood typing reagents to complete, and it takes between 5 and 10 minutes.
However, if you want to test paternity and maternity, you can choose any of the services. They all are simple and effective.
- Eldoncard Blood Type Test (Amazon.com)
- Innovating Science ABO/RH Blood Type Test Kit (Amazon.com)
2. Rh D Antigen
The Rh (for Rhesus) factor or D antigen is a specific blood protein that was found first while investigating Rhesus monkeys.
The majority of people’s blood (almost 80%) contains this protein. However, the protein is absent in some people.
Rh positive refers to persons who have the D antigen, whereas Rh negative refers to those who do not. Negative is recessive while positive is dominant.
Therefore, only Rh-negative offspring will be born to Rh-negative parents.
While Rh-positive parents or one Rh-positive and one Rh-negative can have Rh-positive or Rh-negative children.
Table for Rh D Inheritance in Children From Their Parents
| Parents | Child (possible) | Child (impossible) |
|---|---|---|
| Rh (+) x Rh (+) | Rh (+) , Rh (-) | – |
| Rh (-) x Rh (-) | Rh (-) | Rh (+) |
| Rh (+) x Rh (-) | Rh (+) , Rh (-) | – |
Procedure for Forensic Rh Blood Group Testing:
- To perform the Rh blood grouping procedure, a healthcare provider will typically draw a small sample of blood from a vein in the arm.
- The blood sample is then mixed with reagents that contain antibodies to the Rh factor.
- If the blood sample contains the Rh factor, it will react with the antibodies and form clumps, indicating a positive result.
- If the blood sample does not contain the Rh factor, there will be no clumping, indicating a negative result.
3. MN Blood Group System
Autosomal loci on chromosome 4 regulate the MN blood group, and the two alleles LM and LN are in charge of this blood group.
The presence of glycoprotein on the red blood cell surface identifies this blood group.
The three potential phenotypes are MM, NN, and MN. This is passed down from generation to generation and aids in establishing paternity.
Principle:
The principle of the MN blood group typing test is to determine the presence of M and N antigens on the surface of red blood cells using specific antibodies.
The test involves mixing the patient’s red blood cells with anti-M and anti-N antibodies separately and observing for agglutination (clumping) of the red blood cells.
| Parents | Child (Possible) | Child (Impossible) |
|---|---|---|
| M x M | M | N, MN |
| M x MN | M, MN | N |
| M x N | MN | M, N |
| MN x MN | M, N, MN | None |
| MN x N | N, MN | M |
| N x N | N | M, MN |
Procedure:
- Collect a blood sample from the patient using a sterile needle and syringe.
- Centrifuge the blood sample to separate the red blood cells from the plasma.
- Wash the red blood cells with saline solution to remove any traces of plasma or serum.
- Add a drop of the patient’s red blood cells to separate wells on a glass slide or microtiter plate.
- Add anti-M antibodies to one well and anti-N antibodies to another well.
- Mix the contents of the wells gently and incubate the slide or plate at 37°C for 15-30 minutes.
- Observe for agglutination (clumping) of the red blood cells under a microscope or with the naked eye.
- Record the results as positive or negative for M and N antigens.
Result:
A positive result for the M antigen indicates the presence of the M antigen on the surface of the patient’s red blood cells. While a negative result indicates the absence of the M antigen.
Similarly, a positive result for the N antigen indicates the presence of the N antigen, and a negative result indicates the absence of the N antigen.
Read More: Graham and Margaret Backhouse, Colyn Bedale-Taylor: The Blood Trail Forensic Files Case Study
4. Human Leucocyte Antigen Typing
The identification of HLA antigens forms the foundation of the human leukocyte antigen system.
The HLA test is referred to as a serologic test since it uses antisera (antibodies) to detect antigens.
As genes are inherited from the parents, the chance of paternity is computed using calculations based on the antigens found on the surface of white blood cells.
This test is based on one of two possibilities: (1) Either the man may be excluded ( man is not the child’s father in accordance with genetics), or (2) Inclusion (man might have a genetic background with the child or be the child’s father).
Serological methods used for HLA typing:
Microcytotoxicity Assay
Principle: complement-dependent cytotoxicity -CDC
Lymphocytes are tested with a panel of sera containing well-characterized HLA-specific alloantibodies (immune antibodies that are only produced following exposure to foreign red blood cell antigens).
- HLA class I antigens test: T lymphocytes are chosen
- HLA class II antigens test: B lymphocytes are chosen
Molecular Assays
1. HLA typing using Sequence-Specific Oligonucleotide Probes (SSOP):
Relies on locus-specific amplification of genomic DNA segments comprising the polymorphic sites of HLA alleles.
2. HLA typing using Sequence-Specific Primer (SSP)
Relies on the specificity of primer extension that is matched or mismatched with the template at its 3’end.
A combination of primers designed for polymorphic sequences allows the identification of an allele or group of alleles.
Note: Nucleic acid strands have a directionality, with one end designated as the 3′ (3 prime) end and the other as the 5′ (5 prime) end. In SSP for HLA typing, the 3′ end is significant because the specificity of primer extension relies on the precise matching or mismatching of the primer with the template DNA at this particular end.
3. Sequence Based Typing (SBT)
The polymorphic regions are amplified by PCR and then sequenced. HLA typing eliminates a large number of wrongly accused defendants.
It has been stated that typing for HLA alone provides roughly as much information as can be gathered by investigating all the genetic markers commonly employed in blood tests for paternity.
Read More: Presumptive Blood Tests: 11 Important Forensic Test Included
5. DNA Typing

DNA typing relies on the fact that each individual has a unique genetic code that is inherited from their biological parents.
By comparing the DNA of the alleged father, the child, and the child’s mother (if available), scientists can determine whether the man is the biological father of the child with a high degree of accuracy.
In DNA typing for paternity disputes, scientists analyze specific regions of the DNA that are highly variable between individuals. They include:
A. Variable Number Tandem Repeats (VNTR)
VNTRs (Variable Number Tandem Repeats) are short, repetitive DNA sequences that are highly variable in the number of repeats they contain among individuals.
It is one of the methods for establishing paternity is multilocus DNA fingerprinting because they offer excellent details, somatic stability, and Mendelian inheritance. However, VNTRs are readily replaced with STRs and mini-STRs.
- VNTRs are also known as minisatellites.
- It is composed of repeated units of 10-100 base pairs in length.
- These units are organized in tandem arrays.
- Each variant functions as an inherited allele and can be used for both parental and individual identification.
- Equal VNTR regions in two unrelated people are almost impossible.
B. STRs
Short tandem repeats (STRs), also known as microsatellites, are repeating sequences of DNA that occur at specific locations in the genome.
They consist of a stretch of 2-6 base pairs that repeat in tandem, with the number of repeats varying between individuals.
The three-step procedure involved in STRs:
- During STR analysis, DNA samples from the alleged father, child, and mother (if available) are collected.
- The DNA is extracted from the samples, and specific STR regions are amplified using PCR (polymerase chain reaction).
- The number of repeats for each STR region is determined by analyzing the resulting PCR products using capillary electrophoresis, which separates the PCR products by size.
The resulting data is then analyzed using specialized software to determine the probability of paternity.
The software compares the number of repeats at each STR locus in the child’s DNA to those in the alleged father’s DNA.
- If the child has inherited the same number of repeats from the alleged father at each locus, the probability of paternity is high.
- If the child has a different number of repeats from the alleged father at one or more loci, the probability of paternity is reduced.
Read More: Bloodstain Pattern Analysis: Forensic Types and Classification
6. Types of DNA Markers used in Parentage Testing

A. Autosomal DNA Markers
The examination of the autosomal STR profiling in paternity tests involving a mother, a child, and an alleged father begins with a comparison of the alleles of the mother and child.
This step identifies which of the child’s two alleles is maternal and which is paternal.
B. Y-STR Markers
Along with autosomal STR typing, Y-STR typing is employed as an additional method to establish paternity or to identify specific male sequences in a DNA mixture.
The results of Y-STR typing are interpreted based on haplotype distribution, which exposes the familial relationship pattern due to its uniparental inheritance.
Y-STR Genetic markers can also be used to detect whether two or more male individuals are descended from the same paternal line.
It is based on the genetic fact that the Y chromosome is mainly transferred unmodified from father to son through many generations.
C. X-STR Markers
Males and females both maintain one of their mother’s X chromosomes, and females retain their father’s second X chromosome.
Hence, females with the same male father share their paternal X chromosome, and the other X chromosome is identical to the mother.
As a result, in cases of deficiency paternity where the mother is accessible for typing, it is possible to identify the potential X alleles of the suspected father and reconstruct the paternal profile.
D. Mitochondrial DNA
mtDNA is inherited maternally and is frequently used to trace maternal ancestry. The key benefit is that because:
- mtDNA is present in numerous copies per cell.
- It is generally simpler to obtain enough for examination.
The mt-DNA test establishes whether two people come from the same maternal lineage.
Men and women both receive mitochondrial DNA from their mothers, but only women pass on their mtDNA to their offspring.
The mtDNA test examines the mtDNA sequence on certain non nucleus DNA of the tested parties to see if they are maternally related. mtDNA does not vary significantly from generation to generation.
Procedure for DNA Markers Test:
- To conduct the test, DNA is extracted from the biological samples, such as blood or saliva, of the alleged father, child, and mother (if available).
- The DNA samples are then amplified using PCR, which makes many copies of the DNA/ mtDNA in order to produce enough repeated repeats for analysis.
- The amplified DNA is then analyzed using techniques such as gel electrophoresis, capillary electrophoresis, or next-generation sequencing to determine the genetic profiles of each individual.
If the genetic profile of the alleged father matches that of the child, the probability of paternity can be calculated using statistical methods.
The probability of paternity is typically expressed as a percentage, which indicates the likelihood that the alleged father is the biological father of the child.
Overall, DNA typing is a highly accurate and reliable method for determining paternity/maternity and can provide strong evidence in paternity disputes.
References:
- Mujahid, A., & Dickert, F. L. (2015). Blood Group Typing: From Classical Strategies to the Application of Synthetic Antibodies Generated by Molecular Imprinting. Sensors, 16(1), 51. [DOI]
- Palacajornsuk P. (2006). Review: molecular basis of MNS blood group variants. Immunohematology, 22(4), 171–182.
- Storry, J. (2009). The ABO blood group system revisited: a review and update. Lund University Publications. [link]
- Geserick, G., & Wirth, I. (2012). Genetic Kinship Investigation from Blood Groups to DNA Markers. Transfusion Medicine and Hemotherapy. [DOI]
- Hongbao, M., Zhu, H., Fangxia, G., & Shen, C. (2006). Paternity Testing. Retrieved April 6, 2023, from [Journal]
- Pena, S. D., & Chakraborty, R. (1994). Paternity testing in the DNA era. Trends in Genetics. [DOI]
- Gjertson, D. W., & Morris, J. S. (1995). Assessing the probability of paternity and the product rule in DNA systems. Genetica, 96(1–2), 89–98. [DOI]
- Lee, H. S., Lee, J. W., Han, G. R., & Hwang, J. J. (2000). Motherless case in paternity testing. Forensic science international, 114(2), 57-65.
- Shapiro, E.D., Reifler, S., & Psome, C.L. (1993). The DNA paternity test: legislating the future paternity action. Legal medicine, 233-82.

FR Author Group at ForensicReader is a team of Forensic experts and scholars having B.Sc, M.Sc, or Doctorate( Ph.D.) degrees in Forensic Science. We published on topics on fingerprints, questioned documents, forensic medicine, toxicology, physical evidence, and related case studies. Know More.
